UPDATE 1/10/14 Jahi McMath: A Body in Limbo - by Sprocket
UPDATE 1/6/14: Jahi McMath: Merely Dead, or Really Most Sincerely Dead? by KZ
UPDATE 1/3/14: New story by CaliGirl9 can be found HERE. Sprocket
I have been watching the sad story of Jahi McMath ever since a Facebook friend posted the initial television news story about “how the nurses failed to listen” to “a young girl’s” family’s pleas for help when she started bleeding after a “routine tonsillectomy” for treatment of sleep apnea at Children’s Hospital Oakland (SF Bay area).
Having been an RN and knowing there’s always another side in medicine, I held off the urge to write “Selfish, lazy nurses!” because I know most aren’t. The photo that accompanied the article was of a round-faced, dimpled, smiling young teen who had a very short, heavy neck. I was able to deduce that her sleep apnea was obstructive, not central (in other words, compromised airway instead of defect in the brain).
Media reports from December 15 revealed that Jahi awoke from her “routine tonsillectomy” on Monday, December 9, and was talking, communicating by notes and eating a popsicle the first post-op evening in ICU when “blood started pouring out of her nose and mouth.” The family claims nurses were slow to respond. The family also claims the notes Jahi wrote are missing (though I believe they were probably bled upon and thrown away as medical waste).
Whatever happened, Jahi’s heart stopped beating, either from hypovolemia or aspiration of blood into the lungs, and she was resuscitated and received four transfusions (Via a video, the mother believes her daughter died from “drowning in her own blood. This, of course, is impossible to confirm or deny without an x-ray or an autopsy. Because the hospital cannot release information, we do not know the true cause of her hemorrhage or her heart stopping. Furthermore, if aspiration took place, it may well already be resolved.). She remained unconscious on a ventilator on Tuesday, and at 2 a.m. on Wednesday, signs of hypoxic (lack of oxygen) braininjury via swelling were observed. She underwent a CT scan that revealed 2/3 of her brain had swollen. When the brain swells, it permanently damages neurons, which are the connective sparks within the brain. An excellent tutorial as to what happened is here.
After serial exams, usually performed at least 12 hours apart but preferably 24 hours apart, along with a brain perfusion scan, two electroencephalograms, and five physical exams including an apnea exam, Jahi was declared brain dead on December 12.
Whatever happened, Jahi’s heart stopped beating, either from hypovolemia or aspiration of blood into the lungs, and she was resuscitated and received four transfusions (Via a video, the mother believes her daughter died from “drowning in her own blood. This, of course, is impossible to confirm or deny without an x-ray or an autopsy. Because the hospital cannot release information, we do not know the true cause of her hemorrhage or her heart stopping. Furthermore, if aspiration took place, it may well already be resolved.). She remained unconscious on a ventilator on Tuesday, and at 2 a.m. on Wednesday, signs of hypoxic (lack of oxygen) braininjury via swelling were observed. She underwent a CT scan that revealed 2/3 of her brain had swollen. When the brain swells, it permanently damages neurons, which are the connective sparks within the brain. An excellent tutorial as to what happened is here.
After serial exams, usually performed at least 12 hours apart but preferably 24 hours apart, along with a brain perfusion scan, two electroencephalograms, and five physical exams including an apnea exam, Jahi was declared brain dead on December 12.
Above: Images of normal blood circulation to the brain (left)
and absent blood circulation—brain death (right).
Image from Fusionspark Media Inc.
Per the hospital’s court papers, most families come to terms with the diagnosis, and 2 to 3 days are routinely given for the family to say goodbye. The family did not want Jahi to “die” at Christmas, requested she not be disconnected, asked for 48 hour notice of termination of the ventilator, demanded a “feeding tube,” and began to seek an attorney to force the hospital to keep the teen on the ventilator through Christmas. The media circus and smear campaign against Children’s Hospital Oakland (CHO) began.
Image from Fusionspark Media Inc.
As the days progressed and this what should have been a private tragedy was played out on TV and in newspapers, we were presented with the family’s story of blame toward the doctors and nurses. We read articles where Jahi’s uncle claimed the doctors were heartless and pronounced Jahi “dead, dead, dead.” We came to understand, via a court document from the hospital’s attorney, that Jahi had been examined 5 times by two different neurologists over the course of two days and all exams took the physicians to the same conclusion based on serial EEGs, a brain perfusion scan, physical exams and tests to see if she could breathe on her own (the ventilator is turned off for a short time to see if she takes a breath independent of the machine).
The family was convinced those doctors had an agenda, and that was to kill Jahi. Hence, they scrambled to retain a lawyer (who will remain unnamed because I do not want to contribute to free publicity) and took CHO, an institution with a long history of service to East Bay children and their families, to court, alleging that the hospital wanted to kill Jahi. They asked to have Jahi for Christmas, which would be 13 days after she’d been declared brain dead. Jahi’s body was to be taken off the ventilator sometime after her “last” exam, which occurred on December 16, a week from the surgery and four days after she’d been pronounced brain dead by two different physicians after numerous exams. That final exam was by one of the two CHO physicians.
Because the family was convinced that CHO wanted Jahi dead, even though she’d been pronounced brain dead by two doctors and was, by legal definition, dead, they started a 24-hour vigil at her bedside, to make sure the hospital didn’t do anything behind their backs. They also did not want the ventilator turned off at Christmas time, and they demanded a feeding tube be placed, a request the hospital denied outright, because it does not do procedures on deceased people.
The family was convinced those doctors had an agenda, and that was to kill Jahi. Hence, they scrambled to retain a lawyer (who will remain unnamed because I do not want to contribute to free publicity) and took CHO, an institution with a long history of service to East Bay children and their families, to court, alleging that the hospital wanted to kill Jahi. They asked to have Jahi for Christmas, which would be 13 days after she’d been declared brain dead. Jahi’s body was to be taken off the ventilator sometime after her “last” exam, which occurred on December 16, a week from the surgery and four days after she’d been pronounced brain dead by two different physicians after numerous exams. That final exam was by one of the two CHO physicians.
Because the family was convinced that CHO wanted Jahi dead, even though she’d been pronounced brain dead by two doctors and was, by legal definition, dead, they started a 24-hour vigil at her bedside, to make sure the hospital didn’t do anything behind their backs. They also did not want the ventilator turned off at Christmas time, and they demanded a feeding tube be placed, a request the hospital denied outright, because it does not do procedures on deceased people.
From CHO’s attorney’s response court filings on December 20, we learned that Jahi had not had a simple tonsillectomy, but actually several invasive procedures to open up her upper airway. She’d undergone an adenotonsillectomy, uvulopalatopharyngoplasty, and submucous resection of bilateral inferior turbinates. In laymen’s terms, her tonsils and adenoids had been surgically removed from the back of her throat, her uvula (that thing hanging down at the back of your throat) and soft palate removed or remodeled, and excess soft tissue removed from the back of her nose. These tissues are very fragile and highly vascular, meaning they can bleed a lot, as anyone who has had a nosebleed can testify to. We learned via local media that the teen had recently been given the privilege of taking the bus to nearby Berkeley to get her favorite treat from an ice cream shop: a snickerdoodle ice cream sandwich with vanilla ice cream, despite weight being a huge factor in obstructive sleep apnea.
Via a court order issued December 20, a third physician did a sixth exam without ties to CHO on December 23. Dr. Paul Fisher, pediatric neurologist from Stanford University Hospital, made the same sad diagnosis. In a court order issued on December 23 hours after Dr. Fisher’s exam, Alameda County Superior Court Judge Evilio Grillo made the statement that Jahi had met all of the conditions of brain death and was legally deceased. Before the 6th exam, the mother indicated the family would respect that “non-biased opinion.” The same court order stated the hospital must keep Jahi’s body on the ventilator until 5 p.m., December 30.
Via a court order issued December 20, a third physician did a sixth exam without ties to CHO on December 23. Dr. Paul Fisher, pediatric neurologist from Stanford University Hospital, made the same sad diagnosis. In a court order issued on December 23 hours after Dr. Fisher’s exam, Alameda County Superior Court Judge Evilio Grillo made the statement that Jahi had met all of the conditions of brain death and was legally deceased. Before the 6th exam, the mother indicated the family would respect that “non-biased opinion.” The same court order stated the hospital must keep Jahi’s body on the ventilator until 5 p.m., December 30.
The family moved a Christmas tree into a hospital waiting room and 15 family members celebrated Christmas. There were presents for Jahi, the family played cards and dominoes, and sang Christmas carols at Jahi’s bedside.
Via media reports generated by the family’s attorney or the family themselves during that week, supposedly plans were being made to send Jahi’s body to a long-term care facility, first one in the Bay Area, then one in Southern California. One by one, these unnamed facilities backed out. A church-sponsored fund-raiser was cancelled on December 28. The family set up a GoFundMe account (which now has $41K in it as of this writing) to pay for an air ambulance to take Jahi to a new facility. The family claims a company has been contacted and agreed upon a price of over $20K, but the hospital has yet to hear from it through official physician-to-physician channels. On December 27 the hospital said it would assist in the transfer if certain conditions were met, including the county coroner signing off on the transfer, because Jahi is dead.
Via media reports generated by the family’s attorney or the family themselves during that week, supposedly plans were being made to send Jahi’s body to a long-term care facility, first one in the Bay Area, then one in Southern California. One by one, these unnamed facilities backed out. A church-sponsored fund-raiser was cancelled on December 28. The family set up a GoFundMe account (which now has $41K in it as of this writing) to pay for an air ambulance to take Jahi to a new facility. The family claims a company has been contacted and agreed upon a price of over $20K, but the hospital has yet to hear from it through official physician-to-physician channels. On December 27 the hospital said it would assist in the transfer if certain conditions were met, including the county coroner signing off on the transfer, because Jahi is dead.
In preparation for the “transfer,” the family asked CHO to perform a tracheotomy (where a breathing tube is placed in the larynx for long-term mechanical ventilation) and a gastrostomy tube (where an incision is made into the abdomen through to the stomach and a feeding tube is placed) in preparation for a “transfer.” The hospital refused, saying it was unethical to perform surgery on a dead person.
On December 30 the family claimed to have video proving Jahi was moving. The family claimed to have shown the video to hospital personnel, but a hospital spokesperson stated that spontaneous movement is indeed possible in a brain-dead person. (Not for the faint of heart, but you may Google "Lazarus reflex" and watch a pair of videos to show what might be happening. The family has not released their video to the media.)
Until December 31, no facilities were named. But on that date, a “facility” called New Beginnings in New York said they’d accept Jahi and care for her "as a living person." A quick check reveals a hairdresser and undertaker run New Beginnings on Long Island, and that there is no impatient facility. And probably most disturbing of all, it was revealed that the Terri Schiavo Life & Hope Network had been assisting the family in finding a place for Jahi’s body all along.
Via messages left on SFGate’s message board, commenters claimed that the family did not follow the physician’s post-op instructions. Because of HIPAA laws, the hospital and staff are not allowed to talk, but civilians visiting the hospital are not bound to silence. Numerous posts claimed that the family marched extended family to Jahi’s bedside, talking to her and encouraging her to talk back. Doctors and nurses instructed the parents to keep the teen quiet.
There has also been chatter on message boards regarding co-morbidities. While it is true that anything on the Internet needs to be read with suspicion, sometimes the truth eeks out. Posts were made stating that she had Type 2 diabetes and asthma. Posts were made claiming that Bay Area physicians, when asked by parents about tonsillectomy risks, replied that the word in the medical community was that Jahi’s family failed to disclose a familial predisposition to bleeding. Because of HIPAA laws, the hospital is not allowed to discuss the case at all, and is only allowed to say that Jahi is in the facility and that her condition has not changed.
Things are starting to look like this was family noncompliance, not physician error or nurse negligence. Talking is a no-no in the immediate post-op period after any sort of upper airway surgery. Failing to disclose something as serious as a potential bleeding disorder may well have been fatal.
On Monday December 30, about an hour before the ventilator was to be turned off, Judge Grillo issued another temporary restraining order stating Jahi must be maintained until 5 p.m. on Tuesday, January 7, 2014, and instructed both sides to return with updates—presumably an update from the hospital documenting an unchanged brain status, and the family with a specific facility and legal transport plan. The Superior Court judge refused to order the hospital to the surgical procedures of tracheostomy and gastrostomy. The family attorney also filed in federal court, claiming Jahi’s civil rights was being violated, as well as her rights as a disabled person. The federal court will not hear the case until it has been resolved in the lower courts. The hospital’s attorneys argue that brain-dead deceased people do not have civil rights, nor are they disabled, because they are dead.
On the last day of 2013, 1st District Court of Appeals Judge Robert Dondero instructed attorneys on both sides to submit updates by 4 p.m. on Friday, January 3, 2014, including specifics about a transfer to a long-term facility. In the papers filed with that court, the family attorney’s claimed Jahi’s removal from the ventilator violates her Freedom of Religion and Right to Privacy. The 1st District Court ordered a temporary stay until Tuesday, January 7, 2014.
As of this writing, the hospital has yet to be directly contacted by any licensed facility with a specific transport or admission plan.
In summation, an overweight teenager with other co-morbidities rumored to be Type 2 diabetes, asthma and a familial tendency for bleeding, after two physician opinions, underwent a very extensive remodeling of her upper airway on December 9. She began to bleed for an unknown reason (though some blood loss is common in upper airway surgeries) that evening while in the ICU. For whatever reason, her heart stopped.
In summation, an overweight teenager with other co-morbidities rumored to be Type 2 diabetes, asthma and a familial tendency for bleeding, after two physician opinions, underwent a very extensive remodeling of her upper airway on December 9. She began to bleed for an unknown reason (though some blood loss is common in upper airway surgeries) that evening while in the ICU. For whatever reason, her heart stopped.
It is not known how long doctors worked on Jahi. Standard operating procedure during a code consists of establishing an airway (a nasopharyngeal [into the nostrils and down the throat] or oropharyngeal [in the mouth and down the throat] tube), which is initially ventilated by a bag of oxygen that an RN or respiratory technician operates, chest compressions, and if the cardiac rhythm is favorable, electric shock. A central line may be placed underneath the collarbone into the heart to monitor heart efficiency and blood pressure. Medications are given to restart the heart.
She remained unconscious and on a ventilator all day Tuesday, December 10. In the early-morning hours of December 11, signs of brain swelling were noted. That pressure, combined with a lack of blood flow, effectively killed her cerebral cortex and brain stem. How is it known her brain stem is dead? Because she is unable to breathe on her own without the ventilator, and has no swallow or gag reflex. How do we know her cerebral cortex—the seed of our consciousness and individuality—is dead? She is unconscious because there is no blood flowing through her brain and there is no electrical activity.
Her heart beats because the heart does not need messages from the brain to beat. At the time of the independent physician exam, she was also receiving a medication called Vasopressin, which is used during codes to start a non-beating heart and to maintain heartbeat at the cellular level. Nursing staff in CHO’s ICU are taking care of a deceased person, and a critical care bed is tied up until the ventilator is removed or the body is transferred.
Her heart beats because the heart does not need messages from the brain to beat. At the time of the independent physician exam, she was also receiving a medication called Vasopressin, which is used during codes to start a non-beating heart and to maintain heartbeat at the cellular level. Nursing staff in CHO’s ICU are taking care of a deceased person, and a critical care bed is tied up until the ventilator is removed or the body is transferred.
The family went public on December 16.
For the most non-biased news coverage, I encourage readers to search the Los Angeles Times for its coverage. Most of the coverage garnered in the Bay Area is one-sided, with little investigative work and the family’s statements regurgitated without question.
The title of this piece is “Jahi’s Legacy.” It is sad that this teenager is going to be remembered for her family’s actions through the court. and for the prolonged time her body was kept on a ventilator. What can we learn from Jahi?
First, there is no such thing as foolproof, guaranteed safe surgery. Every surgery carries risks. If a minor is having surgery, the parent must truly understand what is being done, and what can go wrong. In the case of a patient with other health problems, one must know nothing is routine. Asthma by itself was complication enough, but possible Type 2 diabetes and a possible bleeding disorder make surgery very risky.
Second, if surgery is done, post-operative instructions must be followed to the letter. If the patient is a minor, the parent must do their best job in getting the child to adhere. Additionally, a teen should be old enough to follow instructions.
Third, surgery may not be the best way to fix things. How hard did Jahi and her mother try to promote healthy eating and weight loss through exercise? This is probably Jahi’s most important legacy—healthy lifestyles can benefit all of us, and it is up to parents to teach their children. The best way to teach children is by example.
Finally, going to the media may have been intended to garner support and sympathy, but eventually the public tires of a circus. Except, of course, for those on the “Keep Jahi on Life Support” FB page and the GoFundMe website that’s raising money for as of yet non-confirmed air ambulance to an as of yet non-confirmed bona fide licensed medical facility able to care for a dead patient on a ventilator.
I would encourage readers to peruse the court documents for additional information, and to add to intelligent discussion.
What a sad way to start 2014.
LA Times articles on Jahi McMath
Court Documents
12-20-2013 Children's Hospital Opposition to Temp. Restraining Order
12-20-2013 Children's Hospital Physician's Declaration
12-24-2013 Children's Hospital Opposition to Petition to Appoint Dr. Byrne an an Independent Expert
12-27-2013 Children's Hospital Atty Response to family atty
12-30-2013 Children's Hospital - Family Filed Appeal
12-30-2013 McMath Civil Rights Lawsuit Filing
LA Times articles on Jahi McMath
Court Documents
12-20-2013 Children's Hospital Opposition to Temp. Restraining Order
12-20-2013 Children's Hospital Physician's Declaration
12-24-2013 Children's Hospital Opposition to Petition to Appoint Dr. Byrne an an Independent Expert
12-27-2013 Children's Hospital Atty Response to family atty
12-30-2013 Children's Hospital - Family Filed Appeal
12-30-2013 McMath Civil Rights Lawsuit Filing

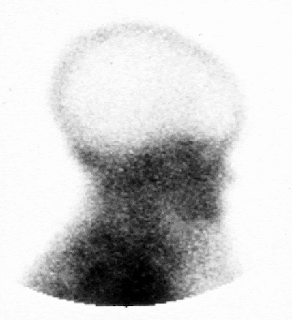






37 comments:
CALIGIRL9, thanks for the well-written summary of what has to be the worst-case scenario. I have followed since the beginning of this child's ordeal and the intervention of all sorts who have an agenda all their own.
From the time she was declared brain dead and the mother and family was given time to peacefully say goodbye to her earthly remains, all I have wondered about was exactly how many children were denied a bed at CHO which could have potentially saved their lives.
Glad to see you here, even with the sad circumstances.
Well done!!!! I am a physician and have been trying to explain all of your above points to people for days. Now I will just refer them to your article.
How will we know that she wont ever wake up if its never been tried before? The fmily are doing a fantastic thing. At least give them a chance and support their wishes.
Perhaps this case will change the way we veiw the term brain dead.
Anon, I am afraid that thousands of previous cases of brain dead/brain stem death sadly prove that what has happened to Jahi is not reversible. All of the anecdotal "I know someone who woke up" probably did NOT receive a diagnosis of brain death via exams, imaging and EEGs and the opinion of three board-certified neurologists. This sets a dangerous precedent in medicine. How many hospitals will be forced to keep brain dead people around until they rot? How many hospitals will not be reimbursed for the cost of warehousing those bodies? How many of those hospitals will go belly-up because they are not only broke, because no insurance cares for the dead? Are taxpayers expected to foot the bill on thousands of hopeless cases? How can anyone believe that at least three doctors wanted to pronounce Jahi dead? I am sure they were looking for the tiniest spark.
The next time this happens—and no doubt somewhere someone has been declared brain dead today—is it a healthy thing for a family to deny the inevitable? So now we have people telling doctors how to practice, even if it is a futile treatment like a gastrostomy tube, which will turn into feces in Jahi's gut, eventually causing skin breakdown because stool will leak and there is simply no way medical staff can stand around waiting for the next ooze to clean it up. She is free to wake up any time she wants or can. She is not receiving any medication keeping her unconscious. Because her cerebral cortex is liquefying, it’s likely there will be more reflex arc movements. Google Lazarus reflex video. Her heart beats because hearts don't need brains in order to beat, they need lungs oxygenating them. What if, when her internal organs breakdown her body develops a bleeding disorder called Disseminated Intravascular Coagulation? She will bleed from every orifice and every pore and it will not be stoppable. Her body temperature will decrease, her blood pressure will decrease, having a negative effect on her kidneys and heart. Her lungs will fill with fluid, there will be cardiac arrhythmias, and diabetes insipidus which will result in high serum sodium and dehydration. Jahi will not feel a thing. Her mother will remember all of it. Did you watch the video? Does the idea of keeping this child's mortal remains on earth long enough to see her brain liquefy sound good? Does the idea of her body leaking stool, or requiring stool to be manually removed from her anus sound appealing? Does the smell of decay appeal to you? Does the idea of bedsores, which WILL happen no matter how good the nursing care is—open, decaying and possibly infected weeping areas of absent flesh exposing the muscle, sinew or maybe even bone beneath—sound pleasant?
Jahi fits every criteria for brain death. Every one. Cannot breathe on her own, no reflexes in her eyes, no purposeful movements from painful stimuli, no gag reflex. Sad but blunt: a deceased person is taking up a scarce resource in the East Bay: a pediatric ICU bed. And what a dangerous precedent we will set when families are allowed to disagree with a policy that is the word of law in this state? How many uninformed people are going to think that the brain heals (which a brain without circulation does not) so all we need is time? During the apnea tests, where the vent is removed to see if Jahi could breathe on her own, doctors would have rejoiced at the tiniest bit of respiratory effort. There was no breathing. The family is unleashing some horrific memories of Jahi on themselves by continuing to deny that she is deceased. Her organs WILL fail and it will be very distressing to watch. Because of the court order, there is no obligation to treat her. A judge has agreed she is dead and the hospital is required only to continue the treatments they'd had in place after she coded—intubated on a ventilator, a urinary catheter, perhaps a subclavian line, and the medication Vasopressin, which is mentioned in the court documents.
Unfortunately, what you have written will never be mentioned to her mother. Or, if it has, she doesn't believe it until she sees it.
This situation is giving me nightmares.
Thank you for taking the time to put this piece together. As a lay person it is very hard to really understand what has happened here. Now that it is clear I am very sad for the family but think she should be laied to rest and her mother begin the grieving process she is so desperate to avoid. I feel very bad also for the doctors and nurses being accused of having an agenda when they did everything they could to help this poor girl and her family.
Excellent article - great explainations-- however, I think we couldve done without the snickerdoodle comment. If she needed such intensive surgery to her pallet/uvula then she most likely needed it regardless of weight. The comment comes off as blaming her for her own death. The doctors shouldnt have performed the surgery if weight loss would have corrected the problem. However, this article is very helpful and answers all related questions. Well done.
What a horror! This should not be allowed to continue. I understand the grief of her family, of course, and a mothers reluctance to let her daughter go. But isn't it time for a funeral already? This is very disturbing indeed.
I have just read a judge has given Jahi s mothet permission to take her daughter from the hospital as long as she accepts full responsibilty for her daughters body. Wow! The horror continues this is very morbid.Her mothers grief must be profound. A part of me wants to say that since the child is deceased she wont keep long on a ventilator anyway,surely she will flatline soon, so whats the harm if that is what it will take to assauge the mothers doubts. But my rational side takes into account all the ghastly side affects that are in store for this family to,deal with as the poor child rots before their eyes. This nightmare is apparantly going to be drawn out to its inevitable, horrid end by this family and I am, horrified at the prospect of a precedent being set here that will have grieving families leeching medical resources to tend to dead bodies on ventilators for indefinite periods of time so they can say goodbye in a way that makes them feel they are somehow warding off a death that has already occured! I find this deeply disturbing. It would be great if that,child made a miracle recovery, but as she is dead, the time for miracles has passed and a funeral would be much more appropriate at this point, and is normally what follows the death of a loved one. Gosh! Ive got a headache!
I see that the hospital has agreed to let the body of Jahi be transferred??? To where? This is obscene.
Cherlyn said:
“Thank you for this article, and Caligirl's comment. I lost my 8 year old niece after a car accident. She was pronounced brain dead within hours. In a situation like this, emotions can get the better of people. I fully understand why this mother would want her child around for Christmas, but I can't fathom why she would want to watch her beautiful daughter's body decompose right in front of her. Her denial is beyond my comprehension.
As far as those making comments about Jahi miraculously returning to her body and coming back to anything resembling life, they simply have never experienced this situation. Jahi is and will continue to be quite an education for them.
Thank you for continuing the education.
Beautiful Jahi is at peace whether we admit it or not. “
###########
YoJoLo said:
CaliGirl9 your article and comment above were very informative and insightful but I have a couple questions. I do not for one second believe that Jahi is alive but how long can a body be kept on a ventilator? Let's say the family goes through with moving her body to a care facility. Despite the bed sores and infection risks, will her body continue indefinitely on a ventilator or will it eventually give up? If it does give up, does it happen over a period of months or years? Is there an answer to that? I tried Googling it up and I can't find if a body can be kept going forever on a ventilator.
Note: I posted these comments that were emailed to me because the individuals were having trouble with the word verification system. I've disabled the verification system, but all comments will still enter a moderation queue before they are approved on the blog. Sprocket.
Could someone explain to me, please, exactly why is it that a brain dead persons body will decay? If she has a heart beat (artificial or not), then blood is still circulating, right? So how is it that she will rot?
CaliGirl9 your article and comment above were very informative and insightful but I have a couple questions. I do not for one second believe that Jahi is alive but how long can a body be kept on a ventilator? Let's say the family goes through with moving her body to a care facility. Despite the bed sores and infection risks, will her body continue indefinitely on a ventilator or will it eventually give up? If it does give up, does it happen over a period of months or years? Is there an answer to that? I tried Googling it up and I can't find if a body can be kept going forever on a ventilator.
I feel very sorry for the family, but, unfortunately, I do not believe either she is still alive but as a parent who knows how I would react. It is easy to say she is costing money, she is this and that..but when it isn't your child..so easy to say..what most are saying.
I really feel for the family and don't wish this to happen even to my worse enemy. Thank you for the article..and of course, the doctors and nurses are not in the profession to kill people. But, I understand how the family is reacting.
May she rest in peace soon.
Very well written. As a medical novice, I appreciate you taking the time to help me understand.
Thank you for some intelligent and heartfelt commentary, which is what I was hoping for.
Cherlyn, I am so sorry for your family’s loss. This whole “brain death/brain stem death” is so hard to understand when it happens to a young person. Eight years is too short for your family to have had your niece. I hope you are all now able to see the good memories when you think of her, and not the horror of the ventilator.
YoJoLo, I am looking for a proper answer to that question. Like everything in medicine, there are few absolutes. I am able to offer this: there was a case somewhere in the U.S. (not the current Texas one) of a family keeping a brain-dead woman on life support for 100 days to ensure fetal viability. Once the woman was disconnected, there was a post-mortem. Her brain was liquefied, scooped out of her skull. The family sued anyway. What you have to remember about that case is the body was receiving medications (mostly hormones) to counteract the absence of pituitary function. The pituitary, of course, is at the base of the brain, and in Jahi’s case, it is dead, too.
I tripped over an article in a British medical journal that discussed the requirements of keeping a brain-dead donor’s body functioning until the organs can be harvested. The immediate post-resuscitation period is one where there is much chaos in the body; that chaos must be managed to keep the organs viable. Jahi did not get that far, nor would any doctor start those medications on a brain-dead person who was not identified as an organ donor.
There have been a couple of tidbits of interest eeking out: (1) This is Jahi’s third surgical attempt to correct sleep apnea; (2) she is incontinent of urine as a consequence of her sleep apnea; and (3) she ha diabetes insipidus, a consequence of the adrenal glands atop the kidneys receiving any feedback from the pituitary, which is, of course, deceased.
And of course, IF the facility in NJ exists, there’s one heck of a storm coming in.
Hoping to do an update tonight once I have more information I can properly disseminate.
Hello Anon @2:22
I am trying to write something that can disseminate that information without being too gross. So if you get grossed out, stop reading.
The fact the brain will turn to goo, proper term “lysis” or “lyse,” is because there is no circulation within the brain. Have you ever heard of a diabetic person losing a toe, foot or leg to circulatory problems? The process is kind of gross… circulation is compromised, the body part goes into vasospasm, less blood is able to enter. Rinse, repeat. Eventually the body part turns black. If you let it go long enough, it rots. Overly simplified, but that’s what is happening to Jahi’s brain.
Other organs will fail because they are not receiving the proper hormonal support. Eventually her heart will have an abnormal rhythm because of electrolyte imbalances, and it will stop.
When a body has been identified as a potential donor, medications are given to keep that hormonal and cardiac support in balance. Because Jahi is not an identified donor, nor would her organs be healthy enough for donation, she is not getting those medications. The vasopressin she was getting at one time will not stop the hormonal or arrhythmia problems.
Thank you for your question.
As this situation drags on I feel less and less sympathetic to this family who is at this point just working the system for their eventual malpractice lawsuit. The child, Jahi is an innocent and my heart goes out to her. I think she had a premonition of her own death but it appears momma knew best.
Such a sad case. Thank you for the information. This should be required reading for nursing and medical students. I was in nursing education for 25 years and the moral/ethical situations have become more complex as we have advanced in knowledge and expertise. I feel very sorry for this family, but sorrier and sadder for this young lady.
Great article, I appreciate your bias toward facts. I am curious on your technical opinion on the case in the link... Could this pregnant woman's body carry a fetus to term? It seems like a pertinent contrast to the tragic case of Jahi, may she be at peace. Wouldnt this pregnant woman's body also detriorate as described above in short course? http://www.cnn.com/2013/12/24/health/pregnant-life-support-texas/
FYI, a California Superior Court is not considered a "lower" court in relation to a federal U.S. District Court. They are both trial level courts.
Excellent article. I now have a much better understanding of this very sad event. This may lead to new laws that protect the deceased.
Is she getting fluid at all? If no fluid it's only a matter of time before she becomes dehydrated and expires in that manner.
I do feel terrible for the parents, it's a tough thing to go through-I had to pull the plug on my mother and more recently on my mother in law. It's never easy, never a cut and dried situation, even if the patient is elderly, or no matter how sick. You keep thinking, "Am I doing everything possible to help my loved one, or am I making a haste decision?" and you also wonder if there is a chance of them recovering. With my mother, a nurse said she had brain stem activity, but she was septic. The doctor had an attitude, yelled at me, and accused me of being immoral. (she had been in the ICU for a week & 1/2 or so. Since nobody had told me there was zero chance of recovery, I figured I was doing the best for her rather than letting her go without trying anything. My MIL I was not so involved with the process, but I was present for the whole 7 days it took. And I often wonder if it's the withdrawing of fluids (and food) that is the actual cause of death.
Where was I going with this? With someone so young I can understand the mother trying anything for her daughter, leaving no stone unturned. But after several doctors declaring her brain dead, it's time to stop.
Extremely well done piece. A tremendous amount of professional knowledge has been put forth here, yet in a way that a non-professional can easily grasp. My heart just aches for this child. She is gone in every sense of the word but for the physical husk she once lived in. I pray the family will just let her go. In no way do I trivialize their loss. To say goodbye to one we love is never easy. Sadly, it feels like their reluctance to do so is more about easing their own guilt, whether real or perceived. And while I don't want to believe that their aim is to profit from this tragedy, the longer this goes on, the more my faith is shaken. My heart also aches for the hospital and staff. This institution and those who work there are dedicated to helping children. Undoubtedly this tragic and grotesque situation is preventing them from doing just that. Tragedy on top of tragedy.
Caligirl9 nice work. Don't think the judge did the right thing here, set things back to the time when we were without the standard of brain death. Have people no idea what it was like then?? Perhaps a few older ICU nurses would like to delve back to that time and relate a story or two to help the public understand why the standard of death is brain death. Others may have better grasp of the way brain death came about. I think the public would benefit from knowing the way it came about. I feel sad about the judges ruling.
As a high risk Labor and Delivery nurse who encountered a case of a brain dead pregnant women, I would seriously doubt the woman in Texas could go to term. The woman in Texas was 14 weeks pregnant when she "died". She is currently 19 weeks pregnant. The body will eventually fail and she is a long way from term. At this point the baby has no chance of viability for another 3 to 4 weeks if then. The women's case I was involved with was about 21 weeks pregnant when she had a brain aneurysm and was declared brain dead but she was kept on life support until her body began to fail due to sepsis. The baby was delivered at about 26 to27 weeks by caesarean section. The baby survived. After the birth the mothers ventilator was discontinued and she was let go.
Thank you for for such a straightforward explanation. It seems somewhat unemotional and fact based.
I find it hard to understand the family's position. I can't tell if they understand the science or are they going more with the religious resurrection angle. Jesus was resurrected in 3 days (right?), so do they really believe their daughter will be resurrected in 21 days.
New post by CaliGirl9 on this story can be found at this link:
The Long, Sad Death of Jahi McMath: The Circus in Okland - There Are No Winners
Hi Anon @9:04
I do believe she is getting IV fluids. Any treatment she was getting after the code has continued. If she is still getting the vasopressin, that goes in very slowly and with a control pump. Some messages left at SFGate indicate she’s on a D5 drip. I am certain she is being hydrated, probably by a peripheral IV.
I am sorry for your family’s losses. Medical science is wonderful, but it can be so cruel.
Hi Anon @9:33
If you have time, or the inclination, I’d love for you to post just how difficult it was to maintain homeostasis in the sad case you worked on. As of now, because Jahi was never considered as a donor, she is not, rightfully IMO, receiving any of those treatments.
And I agree with you about the current case in Texas. I was only paying half-attention. I did not realize they have 5 weeks in the book. Scary that in some medical centers, 20 weeks is considered viable, yet you and I know just how difficult it is to keep a 20-week gestation neonate going.
Thank you for your insightful comments, everyone.
Thank you for writing this and for the comments.
Good facts. However, could have done without the snicker doodle bit. I feel your anger towards the family and your defensiveness as a registered nurse however jahi was a 13 year old girl and no need to put more fault on her now that she is dead. (Or alive as others say.)
What a great article! Fantastic writing and explanations. While I initially felt bad for the family, it now seems a bit of a cash cow. Good to see the facts behind this case and interesting tidbits like the gofundme account. Extreemly enlightening. I'm guessing if this was her third sugery for sleep apnea and that she had diabetes insipidus as well as being obese there needs to be some family responsibility as well. Prevention could have been a key factor here. I have seen a human body decay and it's not pleasant. That smell never leaves you. The ooze of the g-tube site, never heals, it's always open always exuding something until the body rejects the foreign object and creates a crater large enough around it to expell it. Bedsores so large both entire hip joints could be visualized. A bulging anus filled with feces that has to be dug out. Not a pleasant future and certainly not an idea one for a 13 yr old girl. Brain dead or not. I say let her go and let her be at peace. Get back to the business of treating sick kids.
My apologies, I used diabetes insipidus rather than just diabetes. Shouldn't be posting when tired.
Thank you for this excellent piece.
I'm concerned that because of this debacle, other families will feel free to refuse to remove their brain-dead loved-ones from machines. That would impact organ donation and would put a great deal of pressure on hospitals, doctors, nurses, not to mention costs.
As far as the religious angle that figures into this situation, I believe that New York State is the only state that has "reasonable accommodation" on the books vis a vis death and religious beliefs. I'm quite sure that it was added at the request of the Chasidic/Satmar/Ultra Orthodox Jewish community. Jewish Law ("Halakah") defines death as cardiac death, and only cardiac death.
I think blaming a kid and her family for her obesity, and implying that said obesity caused her death and that therefore she and her family are to blame for her death, is indeed a sad way to start 2014. For shame.
The rumored faculty is in NY, not NJ. We(NJ) have our own issues in the media regarding perception.
Otherwise, nice measured and thoughtful analysis and a tragedy that is just like a bad horror or sci-fi movie.
Commenting on this story is now closed. Please comment on the new story, which can be found here:
The Long, Sad Death of Jahi McMath: The Circus in Okland--There Are No Winners
Post a Comment